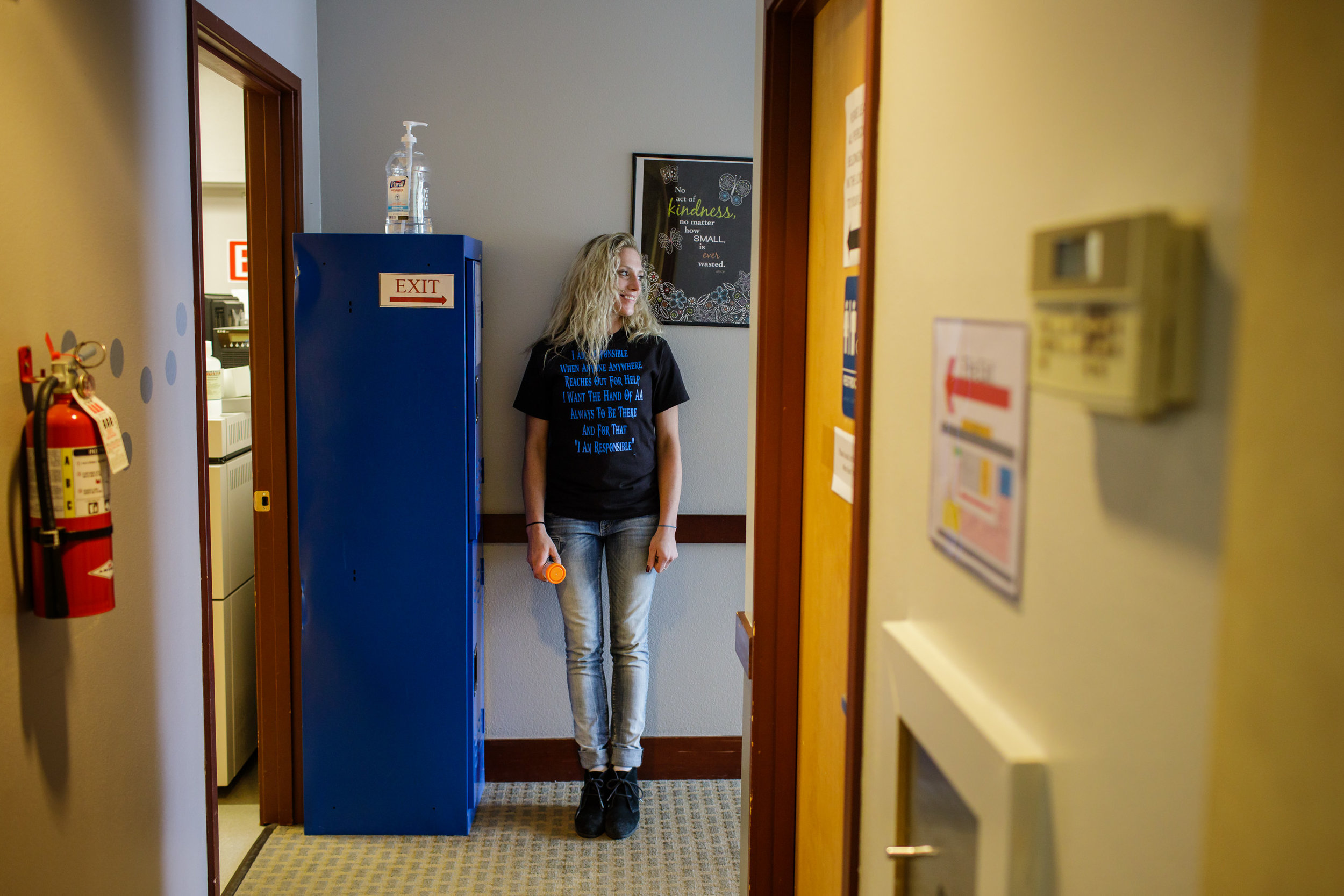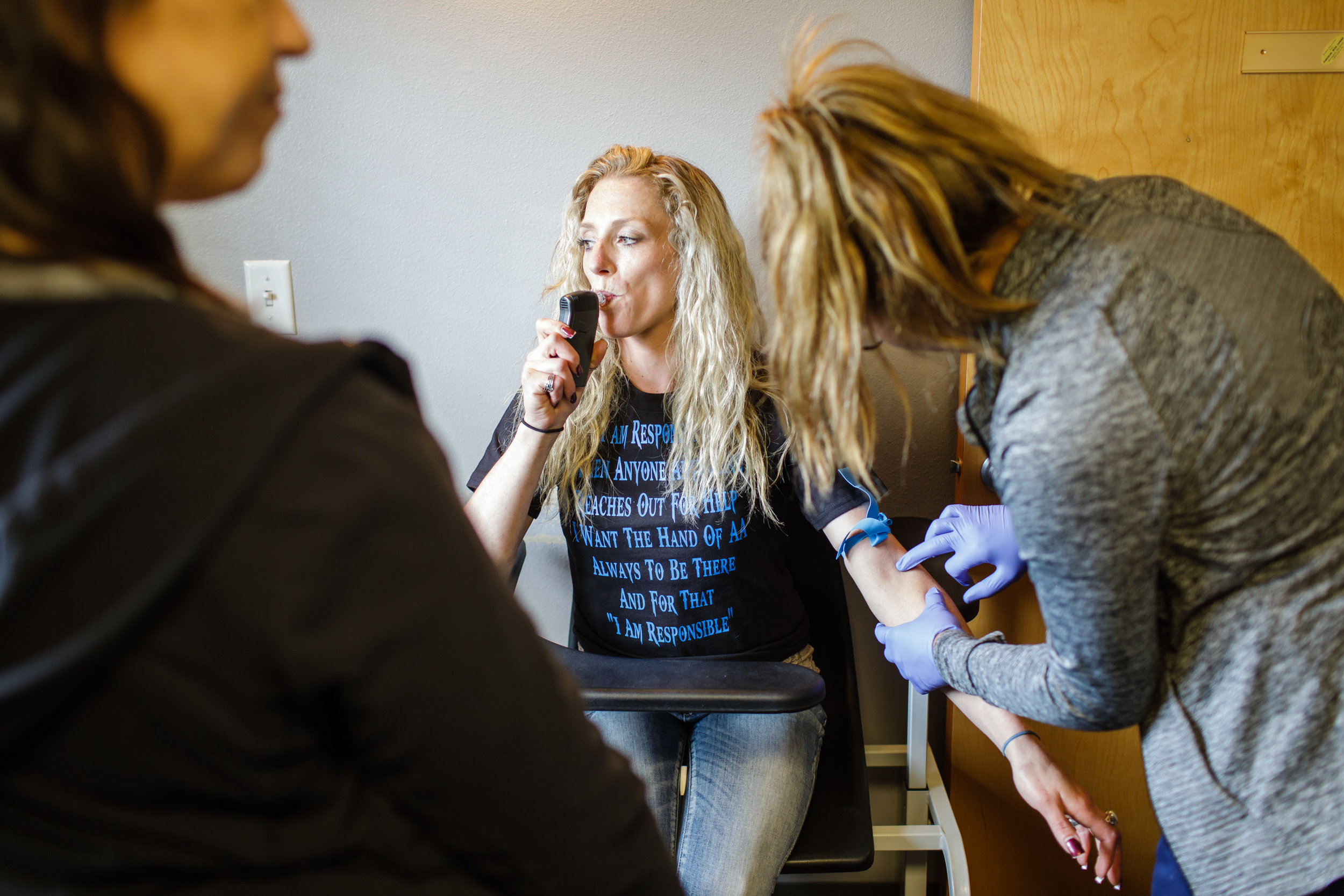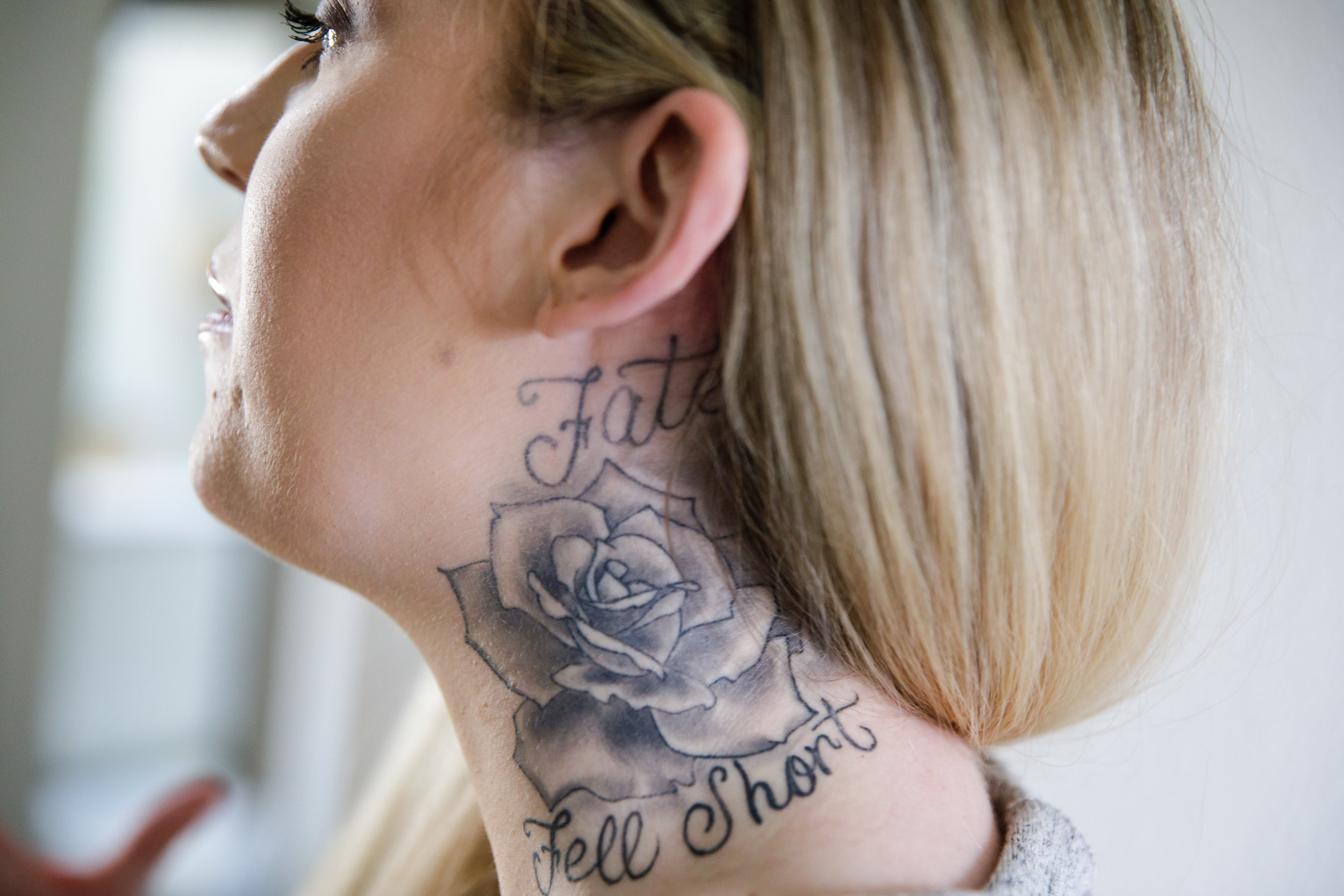Accessible treatment that works
Season 1 Episode 1: Medicine that melts under your tongue
SOLUTION:
Treat addiction using evidence-based medication, like buprenorphine (aka Suboxone). Expand access to treatment through telemedicine.
STORY:
At a clinic in Everett, Washington, a nurse pushes his patients to work hard, and the patients embark on their road to recovery. Do they have a chance? (Yes, and we’ll tell you why.)
This season we’re in Snohomish County, Washington which has an oversized share of overdose deaths in the state and is now treating the opioid epidemic like a natural disaster.
LINKS TO MORE INFORMATION AND RESOURCES:
Snohomish County overdose and addiction treatment resource guide.
Overview of the evidence for medication-assisted treatment (MAT) for opioid use disorders, by the Alcohol and Drug Abuse Institute of the University of Washington.
Research: Buprenorphine is an effective medication that can retain people in treatment.
Research: Patients on buprenorphine were 30 percent more likely to avoid a relapse and 50 percent more likely to stay alive than patients in drug treatment without medication.
Research: Four years after starting Suboxone, over 60% of patients were not using illegal drugs.
TRANSCRIPT
TRANSCRIPT OF FINDING FIXES: EPISODE 1
(Click the play button at the top of this page to listen)
Anna Boiko-Weyrauch: Behind every addiction, there’s pain. That statement became real when we were at clinic in Everett, Washington that treats addiction; it became real when we met one patient, named Ami. She had relapsed on heroin and on this day, she’s thinking of quitting again.
Ami: Which is scary. It’s a scary thought to think about quitting.
Boiko-Weyrauch: But Ami says she’s scared. She speaks in a low voice, and even though we’re all crammed into a tiny exam room, craning forward to hear her, sometimes she’s a little hard to understand
Ami: I used to not feel. A lot of wreckage in my past to have to deal with.
Boiko-Weyrauch: Ami is 32 years old and has been using drugs since she was 12.
Ami: Mostly meth ‘til I was 28, then heroin. Off and on. It is a long time. My teeth are horrible; started falling out. Thank god they’re falling out from the back forward. So the front still looks OK, but this side is getting close.
Ami laughs while talking about her teeth.
Boiko-Weyrauch: Meth is making her teeth fall out. That’s a common side effect. But, she laughs because at least the ones in the back are going first. That’s some dark humor.
Ami really taught me something that day. People who aren’t addicted to drugs, like myself, don’t usually understand something very key to addiction.
Ami is saying once she stops using drugs, that’s when life is going to get hard — she’s going to have to feel.
The drugs are not the problem, it’s the pain of living that’s the problem. And pain is driving this opioid epidemic.
I’m Anna Boiko-Weyrauch.
Kyle Norris: I’m Kyle Norris. We’re radio journalists in Seattle. This podcast is called Finding Fixes. It’s about solutions to the opioid epidemic. That means a few things... looking at how we stop people from getting addicted in the first place; from hurting themselves, their family and friends and communities — and how we stop people from dying.
Each episode we dive into one solution and the people behind it. Those solutions include medical help and counseling, a nose spray that brings people back from an overdose, and taking a good, honest look at all the pain pills that are out there.
Anna and I have spent months getting to know folks in the Puget Sound region connected to this issue. And they’ve let us spend a lot of time picking their brains and following them around. We’ll both take turns hosting this podcast and telling you about the people we’ve met and what they’re doing. Today, Anna takes you there.
Sailboats in Everett, Washington.
CREDIT: LEAH NASH FOR FINDING FIXES »
Boiko-Weyrauch: This episode, we’re in Everett, Washington. It’s just north of Seattle less than an hour away, if there’s no traffic. Just to give you a visual, there are great views of Puget Sound and snow-capped mountains. Seagulls are a constant companion. Boeing builds a lot of planes here.
Two years ago the Los Angeles Times chronicled how black market Oxycontin from LA plunged this city into addiction and heartbreak. The city is also suing Perdue Pharma, which makes Oxycontin.
But in this podcast we're not looking at how the opioid crisis happened, but instead, how to fix it.
A patient waits inside Ideal Option clinic in Everett, Washington.
CREDIT: LEAH NASH FOR FINDING FIXES »
One place that’s trying hard is Ideal Option — it’s a private clinic close to downtown Everett in a tan building. The front door never quite stays closed. The hinge is a little wonky, but also because people are constantly coming in and out.
Patients are coming here to get help treating their addiction to alcohol or opioids.
When they come in for an appointment, they give urine samples to a lab tech who tests it in this machine, they named the machine Vivian. Her job is to find traces of drugs.
And, patients spend some time, with this guy:
Geoff Godfrey is a nurse practitioner at Ideal Option clinic in Everett, Washington. Naturally theatrical, he engages his patients with funny voices and imitations.
CREDIT: LEAH NASH FOR FINDING FIXES »
Norris: And who are you?
Geoff Godfrey: Geoff Godfrey, nurse practitioner, but wait there’s more.
Boiko-Weyrauch: Oh yes, there’s more.
Godfrey: Whaddawe tawking about, fogget it. Don’t go dere.
Boiko-Weyrauch: He does a Brooklyn accent…
Godfrey: Heh, I want my drugs, I want to make you happy!
Boiko-Weyrauch: An imitation of a drug craving…
Godfrey: Yes, beautiful. Yes, quite.
Boiko-Weyrauch: And an opera aficionado. Geoff is so pumped up by his work, the exuberance comes naturally.
Godfrey: I'm really excited about doing this. I was an old E.R. nurse practitioner and this has been the best thing I've ever done in my life.
Norris: Why?
Godfrey: It's healing. You know, so many times we look for a cure but it's the active art of healing, and by engaging these people you really feel like you're part of the therapeutic community… These patients need the help, and then to watch them just get themselves healed. And they do it themselves — they take control back — is just the most amazing thing.
Boiko-Weyrauch: It’s incredible how pumped up he is, because it shows that he’s seen a lot of powerful, positive change in people with addiction.
This transformation comes in part from what’s considered the gold standard in addiction treatment. Treating people addicted to opioids, by using medicine. You might have heard of methadone, that’s one kind of medicine for opioid addiction, and it’s been used for decades.
Maybe you’ve heard of another drug, Naloxone or Narcan. That’s the overdose reversal drug. So that's given to someone who has just overdosed to save their life; lots of paramedics and police officers give it to people. We’re going to talk about Narcan on a different episode.
The medicine at this clinic is Buprenorphine, it also goes by the brand name Suboxone.
A package of the medication, Suboxone, at the Ideal Option clinic in Everett, Wash.
CREDIT: LEAH NASH FOR FINDING FIXES »
Remember these two words because people use them interchangeably. It’s sort of like the words Kleenex and tissues. (Suboxone is the brand name, Buprenorphine is the main ingredient.)
Anyway, Buprenorphine, or Suboxone, comes as a tablet or strip, kind of like a Listerine breath strip that dissolves under your tongue.
Megan Midkiff: When I take the medication I just put it underneath my tongue, and I go about my day.
Boiko-Weyrauch: And such a small thing can be a big boost.
Megan Midkiff lives just south of Everett. She has been on Suboxone for two years. Today she thinks about her two children, her school work, and her friends and church.
When she was on heroin, it hijacked her brain.
Midkiff: It's all consuming, it's all consuming. And that's all you want, all you need and all you're going to do is to get that. Because, at that point, you're just trying to get well. You're not trying to, you know, trying to get high. You're just trying to not be sick.
If someone with an opioid addiction like Megan doesn’t have a steady stream of the drug into their system, they go into withdrawal. Which many people describe as the worst flu you’ve ever had.
Midkiff: I couldn’t take care of my son, I couldn’t talk to any of my friends, I couldn’t work, I couldn’t do anything. It ruined my life. It took everything from me, whereas Suboxone gives me my life.
Boiko-Weyrauch: Now, Megan doesn’t have to worry about withdrawals, because the medication stops those flu-like symptoms and stops cravings.
There is a lot of evidence to back up the effectiveness of this medication and methadone too, by the way.
For example, one study in Massachusetts found people taking the medication were more likely to stay alive and stay off drugs than people in treatment who didn’t use medication. Patients on buprenorphine were 30 percent more likely to avoid a relapse. And this is pretty remarkable: patients on medication were 50 percent more likely to stay alive than patients in drug treatment without medication. 50 percent.
The problem though, is how to get the medication to everyone that needs it.
That’s where clinics like the one in Everett come in.
Patients in front of the Ideal Option clinic in Everett, Wash.
CREDIT: LEAH NASH FOR FINDING FIXES »
Hallie Martin: I usually have really low blood-pressure.
Today, Hallie Martin is coming in for the first time to start treatment using medication.
First, a medical assistant takes her blood pressure, then she leads her to an exam room.
Hallie is 22, she texts constantly with her boyfriend, and sips a red bull Italian soda. (It’s bright turquoise)
Boiko-Weyrauch: Is that your boyfriend?
Martin: Mm-hmm, he’s been blowing my phone up since I got here, I don’t know why.
Boiko-Weyrauch: Later, I find out that she and I were born in the same hospital in Eastern Washington. Sacred Heart.
Subscribe to Finding Fixes on Apple Podcasts
During an appointment, a patient talks to a medical provider through a screen at Ideal Option clinic in Everett, Wash.
CREDIT: LEAH NASH FOR FINDING FIXES »
Payton Drury: Hello.
Hallie Martin: Hi.
Drury: How are you.
Martin: Good, how are you?
Ideal Option is not like any clinic I’ve ever been in. Hallie is going to do an intake interview with a medical assistant on video chat, kind of like Skype. The medical assistant is hundreds of miles away on the other side of Washington state.
Payton: Name, Hallie?
Martin: Yep.
Drury: Just one minute.
Hallie sits in the exam room in a chair facing a large screen with the medical assistant's face on it. There’s a camera to capture Hallie’s face. The word in the medical field of this kind of setup is telemedicine. It’s a way to stretch resources and serve as many patients as possible.
Drury: This is your first ever visit with us, right? What are we seeing you for, alcohol addiction or?
Martin: Opiate addiction.
Boiko-Weyrauch: Payton Drury, the medical assistant asks Hallie a bunch of questions about her addiction, just like she would if they were sitting in the same room.
Drury: and what would you say is your primary substance problem?
Martin: Heroin.
Drury: How would you rate the severity of your addiction on scale of one to ten?
Martin: 11 [laughs]. So a ten.
Boiko-Weyrauch: Hallie has been on opioids since she was 12 years old. That’s when she started on pills. She was smoking heroin at 18 and shooting up at 20. Hallie and the medical assistant cover a lot of ground.
Martin: I suffer from severe depression and anxiety, and a lot of shame and guilt. I have really, like, bad pain though, in my back and in my hips. Cause I used to be a gymnast, and I got hurt.
Boiko-Weyrauch: And starting drinking a lot in high school.
Martin: I drank like probably two or three times a week. I did not keep track. I drank until I was drunk, so however much that took, that’s what I drank.
Boiko-Weyrauch: Hallie says she has a family history of addiction.
Martin: Oh, [snaps] I have severe PTSD. D’uh. Forgot about that.
Hallie Martin poses outside her home in Everett, Wash.
CREDIT: LEAH NASH FOR FINDING FIXES »
Boiko-Weyrauch: All of this history is important. All of these things contribute to addiction.
Let’s just get it out there and say addiction is not a choice. It’s a really complicated disease. And family history, injury, early exposure to drugs and alcohol, mental illness, and trauma play a big, big role. Sometimes it seems so random that some people get really lucky with they hand they’re dealt and never develop an addiction, and some people get really unlucky and face a big struggle.
Payton and Hallie have a lot more questions to get through. On the screen you can see Payton the medical assistant, all the way on the other side of the state, plowing ahead. She removes her cardigan, revealing a sleeve of tattoos.
Martin: I like your tattoos.
Drury: Thank you.
Boiko-Weyrauch: Hallie also has tattoos on her fingers and hands. You can see a big one on her neck with flowers when she pulls back her hair. It reads “fate fell short.”
Hallie Martin's tattoo comes from a Blink 182 song, but also describes her life.
CREDIT: LEAH NASH »
After the questions, the funny nurse practitioner, Geoff Godfrey, comes in.
Godfrey: So! We’re going to get started... What’d I do with my pen? I just left it, I just left it. Oh, look at me. Yeah, I’m an old guy.
Boiko-Weyrauch: Geoff’s about to work his magic with Hallie.
Martin: He’s the funniest doctor I think I’ve ever had.
Norris: Why is that?
Martin: All my other Suboxone doctors are like, a little straight-laced and boring, but you’re not!
Godfrey: But I've got a lousy bedside manner. I warned you right? Because I'm going to hold your feet to the fire. I expect all my patients to engage and love themselves enough to work freakin' hard. I think you’re ready for this.
Geoff and Hallie have met before. Her boyfriend is also a patient here. The couple decided to stop using drugs on Valentine’s Day this year [2018]. It’s March 9th the day we meet her.
Nurse practitioner Geoff Godfrey listens to a patient at the Ideal Option clinic in Everett, Wash.
CREDIT: LEAH NASH FOR FINDING FIXES »
Geoff asks his usual questions.
Godfrey: Are you a shooter or a smoker?
Martin: IV.
Godfrey: Can I see your arms?
Martin: I don’t have any veins. They couldn’t even draw any blood in detox.
Godfrey: Strong work.
Martin: The only vein I have left is my neck.
Godfrey: And when was the last time you shot in your neck?
Martin: February 14th.
Godfrey: Fantastic and you've been clean since?
Martin: February 14th.
Godfrey: Right. That was your last hurrah, wasn’t it?
Martin: Yeah.
Godfrey: Yeah.
Boiko-Weyrauch: But Geoff is hopeful. Recovering from heroin means her body will have a chance to heal.
There’s a good chance the medication will help Hallie.
One long-term study looked at people on Suboxone. It found over 60 percent of patients were not using illegal drugs four years after starting the medication. 60 percent. So this medication doesn’t work for everyone all the time, but it works for a lot of people.
Godfrey: So you’re going to drink 16 to 32 ounces of warm water.
Geoff walks Hallie through how to take it.
He writes down notes for her as he talks. She’s supposed to keep the tablets under her tongue for a little while.
Godfrey: Set your timer for forty minutes, and then you’re going to write out your daily list. Cause you got forty minutes with spit in your mouth, what the heck else are you going to do, right? You’re gonna live your life, right?
Boiko-Weyrauch: Geoff wants patients to start rebuilding their brains too.
Godfrey: Make each thing that you're going to do in your life something that's going to really help you drive you forward.
Boiko-Weyrauch: For Hallie and many other patients, living without drugs means she will need a whole set of different tools to help her get through the day...
Godfrey: So, and counseling, are you already scheduled?
Boiko-Weyrauch: ...help her cope with challenges and pain. Drugs used to be the solution, now she has to rely on other things for support.
Godfrey: Ding the timer goes off, spit that crap out and no smoking an hour afterwards.
Boiko-Weyrauch: One more way this clinic is different from other places.
Godfrey: Siri, please call IO doctor Martin Dubeck. [Siri’s voice]
Boiko-Weyrauch: The actual doctor prescribing the medication isn’t in the office either.
Dubeck: Hiiii!
Dr. Martin Dubeck is about 30 miles north of here in another town.
Dubeck: I’m Dr. Dubeck, my name’s gonna be on your prescription.
Boiko-Weyrauch: There is a reason for this.
Allgaier: The demand is incredible!
Boiko-Weyrauch: We called up the head of the Ideal Option clinic to explain to us how it works. This clinic in Everett is actually part of a network of 36 clinics across eight states.
Dr. Jeff Allgaier is the CEO of Ideal Option. He says there are just not enough doctors to treat everyone who needs it.
Allgaier: Addiction medicine is not something that people go to medical school and say, "I want to practice addiction medicine."
Boiko-Weyrauch: You can also prescribe buprenorphine if you’re a nurse practitioner or physician assistant. But everyone has to take an eight hour course and get a special license.
Allgaier says on top of that, there are federal regulations that limit how many patients providers can prescribe buprenorphine to. These regulations are trying to prevent pill mills.
Allgaier: And pill mills are basically where practitioners will go in and hand out prescriptions, and that’s about all they do. Hand out prescriptions in exchange for money.
Boiko-Weyrauch: Too many drugs handed out without oversight.
Allgaier: Which is one of the issues, the things, the problems that got us into this problem in the first place.
Boiko-Weyrauch: So now, say you’re a doctor or nurse practitioner or physician assistant. You want to help people get off heroin or pain pills and you want to prescribe buprenorphine to help them. You take an eight hour class, you get a federal license. Then, for the first year after that, you can only treat 30 patients. That’s by law. Over time you can go back to the federal government and get permission to treat up to 275 people a year.
The clinic in Everett, though, sees more patients than that in a week.
Allgaier: There is so much more demand for our services than there is a supply of folks being able to provide those services.
So that’s why they use telemedicine. It helps meet that demand.
Dubeck: So, um, let me ask you this...
Dr. Dubeck peers out from the iPhone screen and talks to Hallie. The nurse practitioner, Geoff Godfrey holds the phone and Dr. Dubeck’s face in his hand.
Dubeck: We’re happy to have you and I wish you the best of luck.
Martin: Thank you.
Godfrey: Thanks, Dr. Dubeck.
Dubeck: You’re welcome sir.
Godfrey: Ay ay captain. Ooh, you got the beard going, man.
Dubeck: No, I just didn’t shave. I didn’t shave yesterday.
Godfrey: Ooohhh. I’ll talk to you soon. Thanks sir, bye.
Dubeck: Bye.
Boiko-Weyrauch: Hallie is following a path that others have been down before. Remember Megan Midkiff from earlier in the episode? She’s been on buprenorphine medication for two years.
We should mention one more thing about buprenorphine. It is itself an opioid. For some people, that means, as a treatment for addiction, it’s a nonstarter. It’s pretty polarizing.
Midkiff: If you’re on medication-assisted treatment, you’re not clean in their eyes.
Boiko-Weyrauch: That’s Megan. That stigma comes from surprising place: from within the drug treatment community. Narcotics Anonymous, for example, defines being clean as being totally abstinent from everything, including addiction treatment medication. NA asks people on medication like buprenorphine or methadone to listen at NA meetings, instead of sharing their experiences in front of the group. Megan says that rule isn’t exactly enforced.
Midkiff: I have shared at quite a few meetings where I say it’s hard to not feel "less than," or that I’m not clean, or that I don’t know what freedom tastes like yet.
Boiko-Weyrauch: Megan’s body is dependent on buprenorphine medication. If she doesn’t take it, she will experience withdrawal symptoms.
Midkiff: The sniffles or body aches, dry mouth, headache, sweaty cold chills, and it’ll progressively get worse unless I take my medication.
Boiko-Weyrauch: So you are still physically dependent on an opiate?
Midkiff: Yes, I’m physically dependent on an opiate.
Boiko-Weyrauch: But do you feel addicted?
Midkiff: No not at all.
Boiko-Weyrauch: There’s a big difference, if you follow the clinical definition of addiction. You can find that definition in the fifth edition of The Diagnostic and Statistical Manual of Mental Disorders (people in the field call it the DSM-5).
According to that definition, you have a substance use disorder when you compulsively seek out and use drugs, despite harmful consequences. It interferes with normal life; it causes problems in your life.
That’s not what’s going on with Megan.
Midkiff: I’m in the car by 9:10, every morning.
Boiko-Weyrauch: She drives in traffic, takes her daughter to school, goes to college classes where she’s studying early childhood education.
Midkiff: And when I get out of school, I have about four hours before I have to pick my daughter up. And I usually spend it on campus in the library or the computer lab.
Boiko-Weyrauch: Compare that to what daily life was like when she and her boyfriend at the time were deep in their addiction.
Midkiff: We spent hours, hours, days in a car. When you’re trying to get your drugs, first you’re running around to try and, you know, either pawn or hustle something. And then you’re spending time waiting.
Boiko-Weyrauch: Waiting for the drug dealer.
Midkiff: Yes.
Boiko-Weyrauch: But, the opposite of addiction, isn’t medication. Not according to Megan.
Boiko-Weyrauch: You said something that just like blew me away it was so well said the other day on the phone. That the opposite of addiction is connection?
Midkiff: Yes, the opposite of addiction is connection. If you have a support system, a well-established foundation, you can do anything. That's what you need.
For Megan that's her family and friends, a community through church, her allies at different social services programs. Medication is important, but so is learning to share her feelings.
A tattoo on a patient's hand at the Ideal Option clinic in Everett, Wash.
CREDIT: LEAH NASH FOR FINDING FIXES »
Midkiff: If you're frustrated, you can confide in somebody, you know. I've had to learn how to not shut out my friends. Whenever I was having a hard time I didn't want to bother anybody. I have had to learn to just go ahead and, you know, say it, because they're not going to think I'm stupid. They’re not going to laugh or be annoyed.
Everyone’s path is different. No one treatment works for everyone. Remember Ami from the beginning of the episode?
Ami: I’ve been using drugs since I was twelve.
Boiko-Weyrauch: And how old are you now?
Ami: 32
Boiko-Weyrauch: We caught up with her months later over Facebook. Ami didn’t last long in the Suboxone program. She says she’s still in the same place she was before: afraid to stop using drugs. But soon, she’s going to have to detox. The wreckage of her past is catching up with her in the form of a felony burglary case. Ami is facing prison time.
By contrast, Hallie is ready to start a new chapter and leave drugs behind. She’s done treatment before, she’s relapsed before. This time she wants it to stick.
Martin: I was alive but I wasn't living. I was just surviving and it's not fun. It's like a terrible, like, vicious cycle you get in because then you start to feel, like, all this shame and guilt about doing it, but then you use to cover the shame and guilt up. You just keep going and going and going until you're just completely like dead inside.
Boiko-Weyrauch: Hallie wants to get back to living.
And we’ve reached the end of our episode - focusing on medication and telemedicine to expand treatment for opioid addiction.
Join us next time on Finding Fixes for this story:
Martin: So I, like, did it. And he didn’t really wake up. So I got the other one. He woke up, like jumped up and was like, "What happened?!" And I was like, "I had to Narcan you." And he was like, "Narcan!"
Boiko-Weyrauch: We’ll talk about how to stop death in its tracks.
Kyle Norris: This episode was produced by Anna Boiko-Weyrauch and me, Kyle Norris.
Finding Fixes is a project of InvestigateWest, a journalism nonprofit, reporting on public health, the environment, and government accountability.
Julia Drachman is our producer. Alisa Barba is our editor. Joan Caine is our fairy godmother. Music by Jake Weholt. With help from Paul Keifer and Jarett Jackson. More at www.findingfixes.com.